Client and Family Learning Needs
Infection
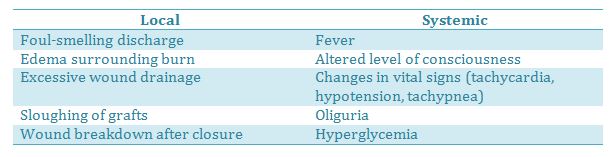
It is imperative that clients and families be knowledgeable about the signs and symptoms of infection, as this is a serious complication that can arise from burn injuries. Signs of infection include:
If a client or family member suspects there is an infection, they should come back to the hospital for management of the infection.
To prevent any infections from occurring it is important to stress good hand hygiene when caring for the burn wounds. Also, some medications can be used to help prevent infections, which will be discussed in the next section.
To prevent any infections from occurring it is important to stress good hand hygiene when caring for the burn wounds. Also, some medications can be used to help prevent infections, which will be discussed in the next section.
Medications
Topical antimicrobials may be used to prevent bacterial growth in wounds that could potentially lead to sepsis. Some of the more common drugs used are silver sulfadiazine (Silvadene) and mafenide acetate (Sulfamylon). These agents may not be used on freshly grafted areas because they inhibit cell growth. Topical antibiotics may be used with the open or closed technique. With the open technique the client or family may clean the wound and apply the cream directly to the burn, while with the closed technique they would clean the wound and then dress it after applying the cream.
Systemic antibiotics may be prescribed when the client has symptoms of an actual infection. Broad-spectrum antibiotics are typically used first until identification of the organism causing the infection is determined.
Pain medications such as morphine sulfate or hydromorphone may also be used depending on the client’s tolerance to pain and any procedures that need to be performed that could cause more pain. If serious procedures such as a fasciotomy are required, anesthetic agents like ketamine and nitrous oxide are used. Teach family members how to monitor for respiratory depression, and the patient how to prevent constipation by drinking fluids and increasing fiber intake.
Nurses should be sure to explain how to use these medications and the side effects of them such as pain or rash from topical agents or nausea and vomiting from a systemic antibiotic. Complimentary and alternative therapies to reduce pain are encouraged so teach the client about different relaxation techniques such as deep breathing and guided imagery, if possible.
Systemic antibiotics may be prescribed when the client has symptoms of an actual infection. Broad-spectrum antibiotics are typically used first until identification of the organism causing the infection is determined.
Pain medications such as morphine sulfate or hydromorphone may also be used depending on the client’s tolerance to pain and any procedures that need to be performed that could cause more pain. If serious procedures such as a fasciotomy are required, anesthetic agents like ketamine and nitrous oxide are used. Teach family members how to monitor for respiratory depression, and the patient how to prevent constipation by drinking fluids and increasing fiber intake.
Nurses should be sure to explain how to use these medications and the side effects of them such as pain or rash from topical agents or nausea and vomiting from a systemic antibiotic. Complimentary and alternative therapies to reduce pain are encouraged so teach the client about different relaxation techniques such as deep breathing and guided imagery, if possible.
Dressing Changes
There are several different types of dressing depending on the type of burn wound including standard, biological and synthetic dressings, and artificial skin. When teaching clients and families how to dress the wounds it is important to not only show them, but also to have them show you so that there is a complete understanding.
For standard wound dressings after they have been cleaned:
As the nurse it is critical to stress the importance of good hand washing to prevent infection in the wounds.
For standard wound dressings after they have been cleaned:
- Apply topical antibiotics if needed
- Add layers of gauze as specified depending on depth and amount of drainage expected
- Use roller type gauze to hold in place wrapping distal to proximal
- Cover wrappings with elastic wraps
- Reapply every 8-24 hours after thorough cleaning
As the nurse it is critical to stress the importance of good hand washing to prevent infection in the wounds.
Maintaining Mobility
While it is important to keep burn wounds dressed and protected from infection, it is also vital to maintain mobility to prevent contractures. Moving joints and ambulating may be painful for burn clients, but it is important to keep good blood flow to aid healing and prevent other injuries. Nurses can educate clients to perform this by using positioning, range-of-motion exercises, ambulation, or pressure dressings.
Range of Motion exercises can be a key factor in maintaining an individual's function which will promote healing, but will also secondary damage caused by muscle atrophy.
Range of Motion exercises can be a key factor in maintaining an individual's function which will promote healing, but will also secondary damage caused by muscle atrophy.
When positioning a client teach the client and family to maintain a neutral position with minimal flexion. There are different position suggestions for different parts of the body that can be found in other resources. For example, to hyper-extend the neck the client can place a towel roll under the neck or to abduct the legs they can place a pillow between the legs. Teach the family how to perform range-of-motion exercises if the client cannot do so to at least three times a day. Ambulation should be performed two to three times a day to strengthen muscles and stimulate immune function, but should only be initiated after fluid shifts have resolved. Pressure dressings are used after grafts, but are fitted in a way that allows mobility and can reduce scarring.